Orthopedic practices across the United States are facing increasing administrative pressure as insurance requirements continue to evolve. In 2026, navigating prior authorization challenges in orthopedic practices and maintaining compliance with modern orthopedic billing guidelines has become a critical part of financial sustainability.
Between complex payer policies, rising denial rates, and increased documentation requirements, orthopedic providers must manage an increasingly demanding billing environment. Without an optimized billing workflow and strong revenue cycle management for orthopedics, practices risk delayed payments, lost revenue, and operational inefficiencies.
This article explores the most common prior authorization challenges in orthopedic surgery, key billing guidelines every practice must follow, and why many providers are turning to outsourcing orthopedic billing services to streamline operations.
Why Orthopedic Billing Is More Complex Than Other Specialties
Orthopedic billing is one of the most complicated areas of medical reimbursement. Procedures such as joint replacements, spinal surgeries, and arthroscopic treatments involve detailed coding structures and strict payer policies.
Following accurate orthopedic billing guidelines requires a deep understanding of:
- CPT procedural coding
- ICD-10 diagnostic coding
- CMS reimbursement policies
- Insurance-specific documentation standards
- Surgical modifier usage
- Global surgical package rules
Because orthopedic surgeries often involve high reimbursement amounts, insurance companies apply stricter claim review processes compared to many other specialties.
Even small billing errors can trigger claim denials or payment delays.
Understanding Prior Authorization in Orthopedic Care
Prior authorization is a process used by insurance companies to verify the medical necessity of certain treatments before they are performed.
Many orthopedic procedures require prior approval, including:
- Knee replacement surgery
- Hip replacement surgery
- Spinal fusion procedures
- Arthroscopic ligament repairs
- MRI and CT imaging
- Orthopedic implants and devices
- Physical therapy services
Although intended to control healthcare costs, prior authorization has become one of the biggest administrative barriers for orthopedic providers.
These prior authorization challenges in orthopedic practices significantly impact both operational efficiency and patient care.
Major Prior Authorization Challenges in Orthopedic Practices
1. Administrative Workload for Medical Staff
One of the most significant prior authorization challenges in orthopedic practices is the heavy administrative burden placed on clinic staff.
Each authorization request requires multiple steps:
- Insurance verification
- Documentation gathering
- Clinical note submission
- Communication with insurance representatives
- Tracking approval status
- Managing denied requests
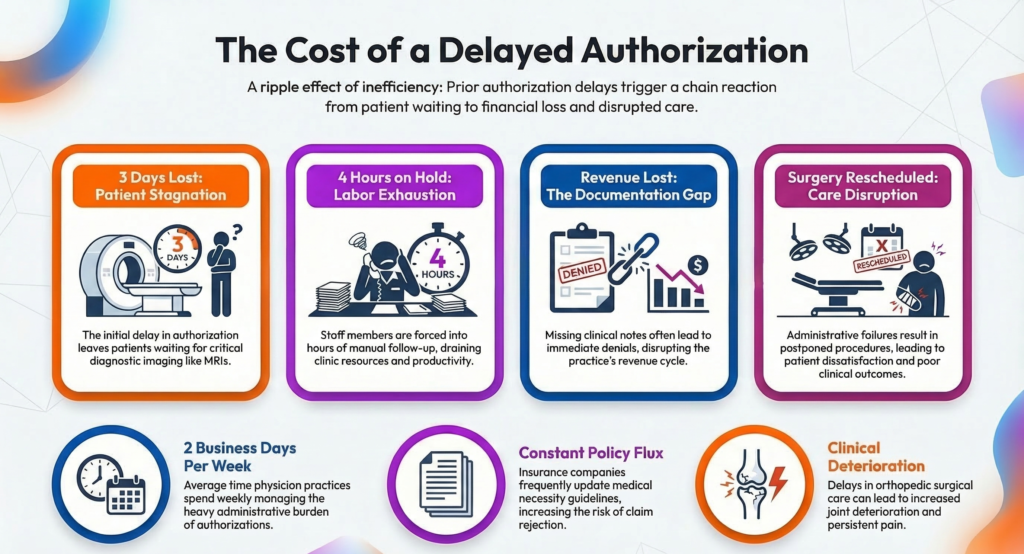
According to the American Medical Association, physician practices spend nearly two business days per week managing prior authorization tasks.
For high-volume orthopedic clinics, this can overwhelm administrative teams.
Stop the Prior Auth Paperwork Drain
Orthopedic practices lose an average of two business days per week to authorization hurdles. Let BillVolt’s RCM experts take the administrative burden off your staff so you can focus on surgery, not phone calls.
2. Delays in Orthopedic Surgical Care
Another major issue is treatment delays caused by slow authorization approvals.
Patients waiting for orthopedic surgery may experience:
- Increased joint deterioration
- Persistent pain
- Reduced mobility
- Prolonged recovery timelines
These delays are particularly concerning in prior authorization challenges in orthopedic surgery, where early intervention can improve surgical outcomes.
Delayed care also affects patient satisfaction and clinic reputation.
3. High Denial Rates for Orthopedic Procedures
Orthopedic claims frequently face authorization denials due to:
- Incomplete clinical documentation
- Incorrect diagnosis coding
- Failure to meet insurer criteria
- Missing imaging reports
Appealing these denials requires additional time, administrative effort, and financial resources.
Without a strong billing system, repeated denials can disrupt the entire revenue cycle management for orthopedics.
4. Constantly Changing Insurance Policies
Insurance companies regularly update their authorization requirements.
Orthopedic practices must continuously monitor changes such as:
- Updated medical necessity guidelines
- New prior authorization rules
- CPT coding updates
- Procedure eligibility requirements
Failing to stay updated on these policy changes increases the risk of claim rejection.
Key Orthopedic Billing Guidelines for 2026
Maintaining compliance with modern orthopedic billing guidelines is essential for reducing denials and maximizing reimbursement.
Below are some critical billing practices orthopedic clinics should follow.
Accurate CPT Coding for Orthopedic Procedures
Orthopedic coding often involves complex surgical procedures that require precise CPT coding.
Common coding challenges include:
- Correct use of modifiers
- Reporting bilateral procedures
- Billing multiple procedures in the same session
- Proper use of add-on codes
Incorrect coding is one of the leading reasons orthopedic claims are denied by insurers.
Strong Clinical Documentation
Proper documentation is essential for supporting medical necessity.
Orthopedic medical records should include:
- Comprehensive patient history
- Physical examination results
- Imaging reports
- Previous conservative treatments
- Detailed surgical indications
- Complete operative notes
Clear documentation improves both authorization approvals and reimbursement accuracy.
Understanding the Global Surgical Package
Many orthopedic surgeries fall under the global surgical package rule, which bundles pre-operative and post-operative care into a single payment.
Billing separately for services already included in the global package can lead to claim denials.
Practices must understand these guidelines to maintain compliance and avoid payment issues.
Strengthening Revenue Cycle Management for Orthopedics
Efficient revenue cycle management for orthopedics is essential for maintaining consistent cash flow and reducing claim delays.
The orthopedic revenue cycle typically includes the following stages:
- Patient scheduling and eligibility verification
- Prior authorization processing
- Medical coding and charge entry
- Claim submission
- Payment posting
- Denial management
- Patient billing and collections
If any step in this process fails, it can disrupt the entire reimbursement cycle.
Strategies to Improve Orthopedic Revenue Cycle Performance
Orthopedic practices can improve financial performance by implementing modern revenue cycle strategies.
Implement Automated Authorization Systems
Technology platforms can track authorization requests, reducing manual follow-ups and missed approvals.
Employ Specialty-Trained Medical Coders
Certified coders with orthopedic experience improve coding accuracy and reduce claim denials.
Monitor Denial Trends
Tracking denial patterns helps identify recurring billing errors and payer policy conflicts.
Optimize Front-End Verification
Accurate insurance verification and eligibility checks can prevent billing errors before services are delivered.
Why Practices Are Outsourcing Orthopedic Billing Services
Due to increasing complexity in orthopedic billing and insurance compliance, many providers now rely on outsourcing orthopedic billing services.
Outsourcing allows practices to focus on patient care while billing experts manage administrative processes. Professional billing providers like BillVolt specialize in handling complex medical billing processes for specialty practices.
How BillVolt Supports Orthopedic Practices
Due to increasing complexity in orthopedic billing and insurance compliance, many providers now rely on outsourcing orthopedic billing services.
Outsourcing allows practices to focus on patient care while billing experts manage administrative processes. Professional billing providers like BillVolt specialize in handling complex medical billing processes for specialty practices.
Access to Specialized Billing Experts
Professional billing companies employ experienced coders familiar with:
- Orthopedic surgical coding
- Modifier application
- Prior authorization workflows
- Insurance policy compliance
This expertise significantly improves claim accuracy and approval rates.
Reduced Administrative Costs
Outsourcing reduces the need for large in-house billing teams, lowering operational costs.
Billing partners handle tasks such as:
- Claims submission
- Authorization tracking
- Payment reconciliation
- Appeals and denial management
Improved Revenue and Cash Flow
Experienced billing companies use advanced tools and analytics to optimize claim processing.
Benefits often include:
- Faster reimbursement cycles
- Reduced claim denial rates
- Improved revenue tracking
- Better financial forecasting
These improvements strengthen overall revenue cycle management for orthopedics.
The Future of Orthopedic Billing and Prior Authorization
Healthcare experts predict that prior authorization processes will continue evolving over the next several years.
However, new technologies may improve efficiency.
Key trends include:
- Electronic prior authorization systems (ePA)
- Artificial intelligence in medical billing
- automated claims processing
- stronger regulatory oversight of insurance companies
These innovations could significantly reduce prior authorization challenges in orthopedic practices.
Conclusion
Managing prior authorization challenges in orthopedic practices has become one of the biggest operational hurdles for providers in 2026. Combined with complex orthopedic billing guidelines, these challenges can affect both patient care and financial performance.
Orthopedic clinics that invest in strong revenue cycle management for orthopedics; whether through improved internal systems or outsourcing orthopedic billing services; are better positioned to reduce claim denials, accelerate reimbursements, and maintain sustainable growth.
In today’s healthcare environment, efficient billing processes are essential for the long-term success of orthopedic practices. At BillVolt, we specialize in revenue cycle management for orthopedics, helping practices streamline prior authorization processes, reduce claim denials, and improve reimbursement timelines. Our team understands the complexities of orthopedic surgery billing, payer policies, and coding requirements, allowing providers to focus more on delivering high-quality patient care.
Whether your practice needs help with prior authorization management, denial resolution, or outsourcing orthopedic billing services, our specialists are here to support your growth and financial stability.
Contact BillVolt today to learn how our orthopedic billing solutions can optimize your revenue cycle and reduce administrative burden.
Stop the Revenue Leak in Your Revenue Cycle
A 10% denial rate isn’t just an “administrative cost” – it’s a direct hit to your practice’s growth. BillVolt specializes in reducing orthopedic denials and accelerating the reimbursement cycle for high-volume practices.
Frequently asked questions (FAQs)
Frequently Asked Questions About Prior Authorization Challenges in Orthopedic Practices
Why is prior authorization so hard for orthopedic surgery?
It’s getting harder because insurance payers now use automated AI models to batch-deny claims that lack specific data. Because orthopedic surgeries (like joint replacements) are high-cost, payers require proof of failure for conservative treatments like PT or injections before they will hit the approve button.
How do I stop Global Period denials in my orthopedic practice?
Most orthopedic surgeries have a 90-day global period. To get paid for a separate service during this time, you must use specific modifiers (like -24 for unrelated visits or -58 for staged procedures). If you don't document the "why" behind the modifier, the claim is automatically rejected as "bundled."
What is the most common reason for orthopedic claim denials in 2026?
The top reason is Insufficient Documentation of Medical Necessity. Payers in 2026 aren't just looking for a diagnosis; they are looking for specific clinical indicators in your operative notes. If your notes don't clearly state the surgical approach (anterior vs. posterior) or the specific anatomy involved, the claim will be denied.
Does every orthopedic procedure need a prior authorization?
Not all, but the list is growing. While office-based injections might not, almost all advanced imaging (MRI/CT) and surgical implants now require a green light from the payer. In 2026, even off-the-shelf orthotics (braces) are being added to the mandatory pre-approval lists for many Medicare Advantage plans.
Can outsourcing my billing actually fix prior auth delays?
Yes, because a specialized partner like BillVolt uses dedicated Auth Specialists who do nothing but track approvals. This stops your front-desk staff from being overwhelmed, prevents surgical day cancellations due to missing auths, and ensures your clean-claim rate stays above 98%.



