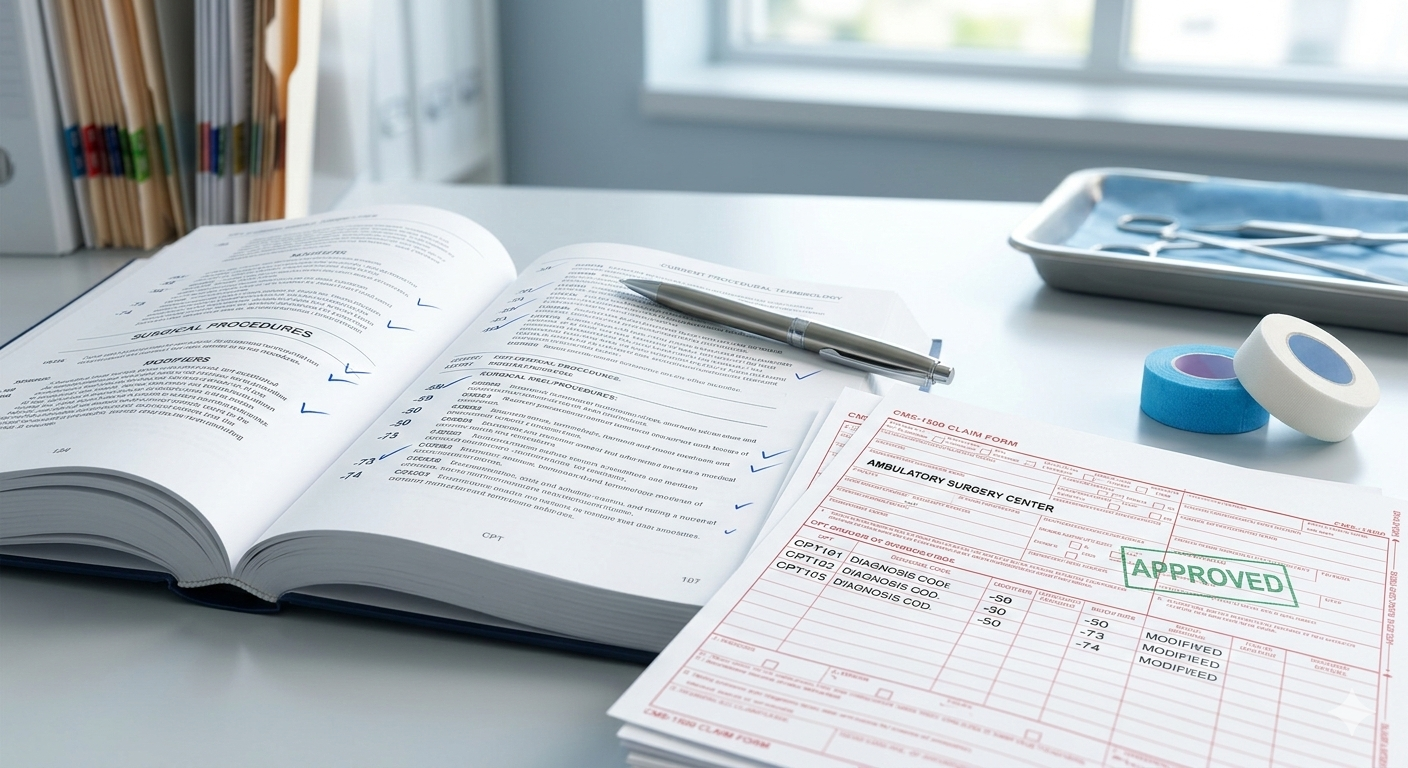
Ambulatory Surgery Centers (ASCs) have become one of the fastest growing segments of the U.S. healthcare system. They offer patients high quality, same day surgical care at a fraction of the cost of hospital outpatient departments. But while ASCs are clinically efficient, billing and coding for ambulatory surgery centers is anything but simple. From CMS regulations and payer-specific rules to modifier usage, bundled services, and documentation standards, ASC billing requires deep expertise. One small mistake can lead to denials, delayed payments, audits, or lost revenue.
This comprehensive guide covers everything ASC administrators, billers, and practice owners need to know about medical billing for ambulatory surgery centers, with a special focus on best coding practices, modifier usage, billing workflows, and revenue cycle optimization.
What is Ambulatory Surgery Center Billing?
ASC medical billing is the process of submitting claims for facility services provided during outpatient surgical procedures. Unlike physician billing, ASCs bill for:
- Use of the surgical facility
- Operating room time
- Medical supplies and surgical equipment
- Recovery room services
- Implants and devices
- Certain diagnostic and technical components
Professional fees for surgeons, anesthesiologists, and pathologists are billed separately.
ASC billing follows a unique reimbursement structure, particularly under Medicare’s ASC Payment System, making accuracy and compliance critical.
Why ASC Billing is More Complex than Traditional Medical Billing
Many healthcare organizations assume ambulatory surgery center (ASC) billing is simply an extension of physician or outpatient billing. In reality, ASC billing operates under an entirely different reimbursement framework, one that is far more restrictive, documentation heavy, and compliance driven.
Below are the key reasons ASC billing is significantly more complex than traditional medical billing, along with real world implications.
Stop Leaving ASC Revenue to Chance
In a system where a single modifier can be the difference between a full payment and a silent denial, close enough isn’t an option. Let our ASC specialists find the hidden gaps in your revenue cycle.
1. CMS-Restricted Procedure Lists
Unlike physician offices or hospital outpatient departments, ASCs are not allowed to bill every surgical procedure. Under Medicare rules, ASCs may only receive reimbursement for procedures included on the ASC Covered Procedures List, which is maintained and updated annually by Centers for Medicare & Medicaid Services.
Why this matters:
- If a procedure is not on the ASC list, Medicare will deny the claim in full, regardless of medical necessity.
- Commercial payers may follow CMS guidelines, but usually apply their own exclusions or limitations.
- Procedures added or removed each year require constant monitoring and updates to coding workflows.
Operational impact:
ASCs must verify procedure eligibility before scheduling surgery, not after. Failure to do so can result in unrecoverable revenue loss.
2. Bundled Reimbursement Models
ASC reimbursement is largely bundled, meaning multiple services are included in a single facility payment rather than reimbursed separately.
In physician billing, services such as:
- Supplies
- Minor procedures
- Certain diagnostics
- Recovery related services
may be billed individually. In ASC billing, many of these are bundled into the facility fee and are not separately payable.
Why this matters:
- Billing bundled services incorrectly can trigger denials or audits.
- Under-bundling leads to compliance risk.
- Over-bundling can hide revenue opportunities for payable add-on services.
Operational impact:
ASC coders must understand what is included, what is excluded, and what qualifies for separate reimbursement, which varies by payer and procedure type.
3. High Modifier Dependency
Modifiers play a much larger role in ASC billing than in standard medical billing. They communicate critical information about:
- Whether procedures were distinct
- If services were reduced or discontinued
- Whether procedures were bilateral
- The technical vs professional components of care
In many ASC claims, reimbursement accuracy depends more on correct modifier usage than the base CPT code itself.
Why this matters:
- Missing modifiers often lead to silent underpayments, not outright denials.
- Incorrect modifier usage increases audit risk.
- Payers apply strict bundling edits that can only be overridden with proper modifier justification.
Operational impact:
ASC billing teams must apply modifiers with surgical level precision, supported by detailed operative documentation, not assumptions.
4. Strict Documentation Requirements
ASC billing lives and dies by documentation. Payers expect clear, consistent, and comprehensive operative reports that justify every billed service.
ASC documentation must support:
- Medical necessity
- Procedure selection
- Modifier usage
- Laterality and anatomical site
- Use of implants and devices
- Discontinued or reduced services
Why this matters:
- Even correctly coded claims can be denied if documentation is insufficient.
- Documentation inconsistencies between facility and professional claims raise red flags.
- Audits often focus on operative notes rather than codes alone.
Operational impact:
ASCs must enforce standardized documentation protocols and ensure providers understand how their notes affect reimbursement.
5. Dual Claim Coordination (Facility vs Professional Billing)
ASC billing involves two parallel but interdependent claims:
- The facility claim (ASC services)
- The professional claim (surgeon, anesthesia, pathology)
Although submitted separately, payers frequently compare them for consistency.
Why this matters:
- Mismatched CPT codes, dates, modifiers, or diagnoses can trigger payer reviews.
- Discrepancies often result in delayed payments or requests for records.
- Poor coordination increases denial rates and days in A/R.
Operational impact:
ASC billing teams must maintain tight alignment between facility and professional billing workflows, even when different entities handle each claim. ASC billing is not “just outpatient billing.” It is a highly regulated, procedure driven, modifier dependent reimbursement system with little margin for error.
Without ASC-specific billing knowledge, surgery centers face:
- Increased denials and underpayments
- Compliance risks and audits
- Delayed cash flow
- Lost revenue that is difficult to recover
This is why successful ASCs rely on dedicated ASC billing and coding expertise, rather than generic medical billing processes.
The ASC Revenue Cycle: Billing & Coding Breakdown
An optimized ASC revenue cycle is proactive, not reactive. Each phase plays a role in reducing denials and maximizing reimbursement.
Pre-Registration & Insurance Verification
Before surgery, confirm:
- Active insurance coverage
- ASC eligibility
- Deductibles and copays
- Prior authorization requirements
Failure at this stage often leads to avoidable denials.
Charge Capture Best Practices
Accurate charge capture ensures nothing is left on the table. Every ASC case should include:
- Primary procedure codes
- Add-on procedures
- Supplies and disposable items
- Implants and devices
- Anesthesia time documentation
Missed charges = lost revenue
ASC Medical Coding: Best Practices
ASC coding is not generic outpatient coding. It requires specialization.
Use Only ASC-Approved CPT Codes
Always verify that procedures are reimbursable in an ASC setting especially for Medicare patients.
Match ICD-10 Codes to Medical Necessity
Diagnosis codes must justify the procedure. Incorrect ICD-10 selection is a leading cause of denials.
Avoid Over-Coding and Under-Coding
- Over-coding increases audit risk
- Under-coding results in revenue loss
Accuracy matters more than volume.
Top Procedure Categories Commonly Billed by ASCs
While codes vary by specialty, ASCs frequently bill procedures in these areas:
Orthopedics
- Arthroscopic knee and shoulder surgeries
- Meniscus repairs
- Ligament reconstructions
Gastroenterology
- Colonoscopies and upper endoscopies
- Polypectomies
- Biopsies
Ophthalmology
- Cataract extractions
- Lens implants
- Retinal procedures
Pain Management
- Epidural injections
- Nerve blocks
- Radiofrequency ablations
ENT
- Sinus surgeries
- Tonsillectomies
- Ear tube placements
Each specialty has unique bundling and modifier rules, making specialization essential.
Modifier Usage: One of the Most Critical ASC Coding Elements
Modifiers tell payers how a procedure was performed. Missing or incorrect modifiers lead to underpayment rather than outright denial, making revenue loss harder to detect.
Most Important Modifiers in ASC Billing
Modifier -SG
- Identifies services performed in an ASC
- Commonly required on facility claims
Modifier -59 (Distinct Procedural Service)
- Indicates procedures were separate and independent
- Used to bypass bundling edits
Should be used sparingly and only when documentation supports it
When possible, use X modifiers (XE, XS, XP, XU) for greater specificity
Modifier -50 (Bilateral Procedures)
- Indicates procedures performed on both sides
- Some payers require two separate line items instead
Modifier -52 (Reduced Services)
- Used when a procedure is partially completed
- Common in GI cases
Clear documentation is mandatory.
Modifier -73 / -74
- Used for discontinued procedures
- Payment depends on when the procedure was stopped
Incorrect use can significantly reduce reimbursement.
ASC Documentation Standards that Support Clean Claims
Coding is only as strong as the documentation behind it. Every operative report should clearly include:
- Pre- and post operative diagnoses
- Detailed procedure narrative
- Anatomical site and laterality
- Anesthesia type and duration
- Implants, devices, and serial numbers
- Reason for discontinued procedures
Incomplete documentation is one of the top causes of ASC claim delays.
Best Billing Practices for Ambulatory Surgery Centers
Strong billing practices ensure fast, accurate reimbursement.
Submit Clean Claims the First Time
- Validate patient demographics
- Confirm coding and modifiers
- Review payer-specific rules
Clean claims get paid faster.
Monitor Denials Aggressively
Common ASC denial reasons include:
- Non-covered procedures
- Missing modifiers
- Lack of medical necessity
- Authorization issues
Tracking denial trends helps prevent repeat errors.
Appeal Underpayments
Many ASC claims are underpaid rather than denied. Without proper follow-up, revenue is silently lost.
Maintain Compliance & Audit Readiness
Regular internal audits reduce:
- Compliance risk
- Overpayment recoupments
- Medicare and commercial payer penalties
Why Many ASCs Outsource Billing and Coding
Because of the complexity involved, many ASCs partner with specialized billing companies to:
- Reduce operational overhead
- Improve cash flow
- Ensure coding compliance
- Handle denials and appeals efficiently
At BillVolt, we specialize in ASC medical billing and coding, offering:
- Certified ASC coders
- Modifier accuracy reviews
- End-to-end revenue cycle management
- Detailed financial reporting
👉 Learn more about our medical billing services.
👉 Explore our medical coding expertise
Turning ASC Billing into a Competitive Advantage
Medical billing for ambulatory surgery centers is complex; but when done right, it becomes a powerful driver of financial success.
By focusing on:
- Accurate coding
- Proper modifier usage
- Strong documentation
- Proactive billing workflows
ASCs can achieve:
Faster payments
Fewer denials
Higher reimbursement per case
Lower audit risk
More focus on patient care
Whether you manage a single ASC or multiple locations, investing in the right billing and coding strategy is no longer optional, it’s essential.
Ready to optimize your ASC revenue cycle?
Visit BillVolt and schedule a free consultation with our billing experts.